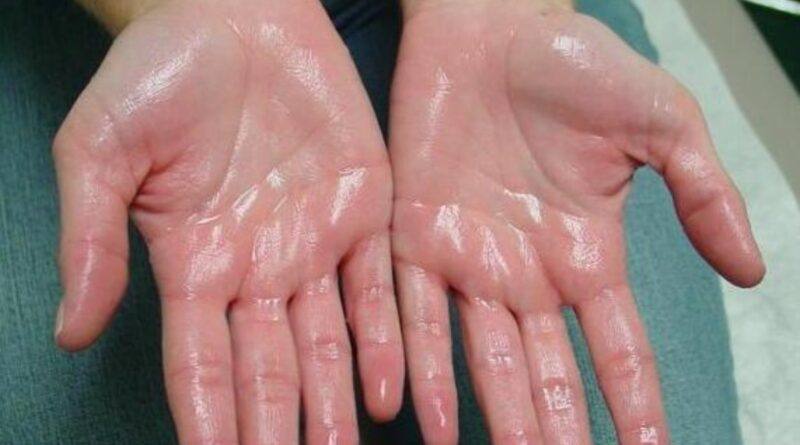
Hyperhidrosis: Amazing Way To Overcome A Rare Sweat Disorder
Health & Wellness · The WFY · June 2025 WFY Bureau Desk
Hyperhidrosis Unmasked: Understanding Excessive Sweating and How to Tame It — A Guide for the Global Indian Community
1 | Why talk about sweat?
A sheen of perspiration during a Kolkata summer or a brisk walk in London’s Hyde Park is perfectly normal. Sweating is the body’s in-built air-conditioning, keeping core temperature within a safe band of 36-37 °C. For roughly 5 percent of the world’s population—around 390 million people—this physiological drip-feed becomes a torrent. Shirts soak through, handshake anxiety rules meetings, sandals become slippery, and nightclothes need daily washing. The medical name for this phenomenon is hyperhidrosis: sweating in quantities far beyond what temperature control requires.
For Indian-origin people dispersed across humid tropics, arid deserts, and air-conditioned offices alike, hyperhidrosis can dent confidence, limit career choices (think surgeons, musicians, IT professionals handling devices), and even threaten mental health. Yet few seek help; in one UK study, only 38 percent of sufferers had spoken to a clinician, largely because they assumed nothing could be done.
This feature sets out to change that assumption. We explore:
- The physiology and two main forms of hyperhidrosis
- Hidden triggers ranging from thyroid imbalance to spicy snacks
- Evidence-based lifestyle tweaks and home strategies
- Medical interventions—from aluminium chloride rolls-ons to microwave thermolysis
- Specific cultural and climatic considerations for the Indian diaspora
By the final paragraph you should possess a practical action plan—whether you sweat through your kurta in Mumbai, fog your spectacles in Toronto, or worry about body odour on the Dubai Metro.
2 | Sweating 101: a crash course in eccrine and apocrine glands
Human skin houses two chief sweat-making units:
- Eccrine glands (about 2 – 4 million scattered over the body) excrete a clear, odourless, watery fluid directly to the skin surface. Their prime directive is temperature control.
- Apocrine glands, heavily concentrated in the underarms and groin, produce a thicker fluid rich in proteins and lipids that bacteria love—hence characteristic body odour.
In hyperhidrosis, eccrine glands are the usual culprits, although apocrine overdrive can worsen odour.
3 | Primary versus secondary hyperhidrosis: spotting the difference
3.1 Primary (focal) hyperhidrosis
- Definition: Excess sweating without an underlying medical illness.
- Pattern: Localised to one or more regions—palms, soles, underarms, face, or groin.
- Onset: Often in childhood or adolescence; up to 65 percent report a positive family history, implying genetic predisposition.
- Triggers: Heat, stress, caffeine, or sometimes no trigger at all.
- Impact: Routine tasks—typing, driving, holding hands in prayer—become fraught.
3.2 Secondary (generalised) hyperhidrosis
- Definition: Excess sweating caused by another medical condition or a drug side-effect.
- Pattern: Typically whole-body, including night sweats.
- Common causes:
- Overactive thyroid (hyperthyroidism)
- Menopause (hot flushes)
- Low blood sugar (hypoglycaemia)
- Obesity
- Infections such as tuberculosis or malaria
- Certain prescriptions (selective serotonin re-uptake inhibitors, antipyretics like paracetamol)
- Neurological disease or injury (Parkinson’s, spinal cord trauma)
Persistent, sudden-onset, or nocturnal sweat storms demand medical appraisal to rule out secondary drivers.
4 | When is sweat too much? Red-flag indicators
- Soaking through two or more shirts daily despite mild weather
- Visible dripping from palms or forehead during sedentary tasks
- Slippery steering wheel or phone due to hand moisture
- Foot odour severe enough to notice through shoes
- Chronic skin infections (athlete’s foot, intertrigo) in damp areas
- Emotional distress, social withdrawal, or occupational impairment
If these resonate, a GP appointment is prudent. Basic work-up may include thyroid function tests, fasting blood glucose, haemoglobin, and medication review.
5 | Home and lifestyle measures: first-line defence
5.1 Hydrate intelligently
Counter-intuitive as it sounds, adequate water (2–2.5 L daily) lowers core temperature, reducing the amount of sweat required for cooling. Coconut water, buttermilk, or oral rehydration salts replace sodium, potassium, and magnesium lost in profuse perspiration.
5.2 Electrolyte-balanced diet
- Potassium (bananas, spinach) helps cellular fluid balance.
- Magnesium (almonds, leafy veg) modulates sympathetic nerve activity.
- Calcium (dairy, ragi) participates in neuromuscular signalling; deficiency may heighten sweat response.
5.3 Clothing calculus
Breathable fabrics—cotton, bamboo, modern moisture-wick synthetics—release steam faster than silk, rayon, or tight polyester blends. Light colours reflect solar radiation; loose weaves promote airflow.
5.4 Antiperspirants versus deodorants
- Antiperspirants contain aluminium chloride or zirconium salts that plug sweat ducts. Look for ≥ 15 percent aluminium chloride hexahydrate in OTC roll-ons; apply at night to dry skin.
- Deodorants only mask odour. In hyperhidrosis, opt for combination “antiperspirant deodorants”.
5.5 Talc, starch, and clays
Dusting powders (zinc oxide, arrowroot) absorb moisture and minimise friction. Use sparingly to avoid caking.
5.6 Caffeine, alcohol, chilli moderation
These substances stimulate sympathetic nerves and heat production. Anecdotally, trimming coffee to ≤ 200 mg/day (about two cups) and limiting spicy dinners reduces flare-ups.
5.7 Stress-management routines
Meditation, pranayama, tai-chi—all lower sympathetic hyperarousal. A 2019 Indian Institute of Mental Health study reported a 22 percent reduction in palmar sweating after eight weeks of daily 15-minute deep-breathing practice.
6 | Medical and procedural options: when DIY is insufficient
| Intervention | Indication | Efficacy & duration | Caveats |
| Prescription-strength aluminium chloride (20–30 %) | Underarm, palm, sole | 60–90 % improvement; nightly for 1 week then maintenance | Skin irritation; apply on dry nights |
| Iontophoresis (tap-water electric current bath) | Palms, soles | 70 % dryness; sessions 2-3 times/week then weekly | Slight tingling; not for pacemaker users |
| Botulinum toxin A injections | Underarm, forehead, palms | 80–95 % reduction; lasts 4–8 months | Discomfort, cost; temporary grip weakness |
| Glycopyrronium or oxybutynin oral tablets | Generalised or multifocal | 50–70 % relief | Dry mouth, blurred vision; needs monitoring |
| Microwave thermolysis (miraDry®) | Axillary glands | Permanent 80 % sweat reduction | Swelling, rare nerve pain; costly |
| Endoscopic thoracic sympathectomy | Severe palmar hyperhidrosis unresponsive to other treatment | Immediate near-total dryness | Risk of compensatory trunk sweating; surgery only as last resort |
Consult a dermatologist or neurologist before starting these therapies; suitability varies by age, health, and sweat map.
7 | The diaspora dimension: climate, culture, career
7.1 Tropical childhood, temperate adulthood
Many Indians raised in hot, humid climates have high baseline sweat rates. Immigrating to colder nations may mask hyperhidrosis for months, only for it to roar back during summer or indoor heating season. Recognising cyclical patterns aids planning—carry spare shirts, pocket antiperspirant, or schedule iontophoresis top-ups before travel to sultry regions.
7.2 Religious and social rituals
From Namaste hand greetings to gurudwara volunteer work requiring stainless-steel bowls, soggy palms can undermine confidence. Open conversation with family and community can reduce stigma and facilitate practical adjustments—e.g., using disposable food-service gloves during seva.
7.3 Technology sector realities
Extended keyboard use worsens palmar moisture, risking device slippage or trackpad malfunction. Silicone keyboard covers, absorbent desk pads, and matte phone grips offer inexpensive mitigation.
8 | Children and adolescents: spotting the signs early
Signs include reluctance to hold pencils, smudged schoolwork, avoidance of sports due to slippery grips, or refusal to join group photos. Paediatric dermatologists recommend starting with aluminium chloride wipes and iontophoresis; early intervention prevents social anxiety.
9 | Myth-busting corner
| Myth | Reality |
| “Hyperhidrosis sufferers are just anxious people.” | Anxiety can trigger sweating but is not the root cause of primary hyperhidrosis. |
| “Drinking less water stops sweating.” | Dehydration stresses the body, often increasing temperature and sweat production. |
| “Natural remedies like apple-cider vinegar cure the condition.” | Limited evidence; may complement but rarely replace medical approaches. |
10 | A 30-day perspiration-proof plan
Week 1: Daily diary—log triggers, sweat scale, foods.
Week 2: Introduce 20 % aluminium chloride nights; switch to cotton layers; begin 10-minute pranayama.
Week 3: Schedule dermatologist tele-consult if < 50 % improvement; trial iontophoresis or prescription anticholinergic.
Week 4: Re-assess; celebrate wins (dry handshake, odour reduction). Adjust maintenance routine for long-term control.
11 | Looking ahead: research on the horizon
- Topical botulinum toxin creams undergoing Phase II trials promise needle-free relief.
- Gene-editing insights into the sympathetic cholinergic pathway may yield precision therapies.
- Wearable sweat sensors could objectively track treatment response, guiding personalised regimens.
The future is optimistic—hyperhidrosis may soon be as manageable as allergic rhinitis or acne.
Reclaiming comfort, confidence, and community
Hyperhidrosis is neither rare nor trivial. For millions—including a substantial share of the Indian diaspora—it blurs the joy of everyday human interaction. The cascade from damp palms to dampened spirit is avoidable. By blending ancestral wisdom (breathwork, herbal dusting powders) with 21st-century dermatology, sufferers can exchange embarrassment for empowerment.
Remember: sweat is natural; excessive sweat is medical—and medicine has answers.
Disclaimer: This article offers general educational information and should not replace professional medical advice. Always consult a qualified healthcare practitioner before beginning new treatments or if you notice sudden or severe changes in sweating patterns.
© 2025 The WFY Magazine. All rights reserved.